‘We can’t help everybody’
As homebirth requests spike, midwives tell some moms they’d be better off at the hospital



Rebecca Azzi was planning to deliver her third baby, due April 7, at St. Anthony Community Hospital in Warwick, NY, with her husband and doula and no drugs, just as she’d done with her first two.
But with the pandemic gathering steam and hospital rules tightening in response, Azzi grew increasingly uneasy. On top of the disquiet of “bringing new life into this world where you have to wear a mask,” she said, there were the twin anxieties about having to go out and interact with a lot of people at a hospital, and having to labor without the support she’d been expecting.
Less than a month before her due date, she called the midwife – whom she’d met with early on in this pregnancy, when she had briefly considered a home birth – to ask if she would be “kind of a backup for us if things got tighter.”
Azzi had come to terms with the idea that her doula would not be at this birth – “that was a loss,” she said. But when New York hospitals banned partners from delivery rooms, “that was the breaking point for us. I could not imagine giving birth without support.” She called the midwife and told her, “We would like to lock in our decision with you.”
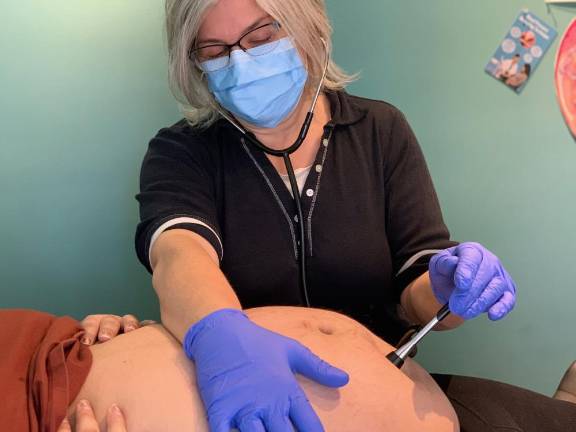
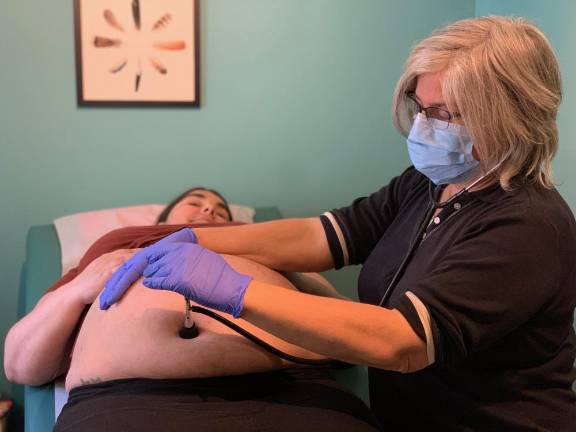
Susan Rannestad, of New Paltz-based River and Mountain Midwives, took Azzi on. She drove to the Azzis’ house in Chester to deliver a birth kit and a birthing tub, check on the mom and the fetus, and sit with the couple and their doula in the living room, going over the day-of details. Everyone was wearing N95 masks and sitting as far apart as possible. “It was very surreal,” said Azzi. “But still, very comforting. I felt a lot more at peace after she left. I just felt okay, he is coming one way or another, and I have an amazing team to help me make that happen.”
Interest in homebirth has been tracing a curve in parallel with the coronavirus. In mid-March, midwives started getting cold calls to their closely guarded personal numbers, sometimes at 3 a.m., from expectant moms who didn’t understand that homebirth midwives never turn off their phones. Then when the ban on partners in delivery rooms was announced on March 18, that was when midwives’ phones – retired or not, in-state or not – starting ringing off the hook.
For those three days when expectant moms were facing the prospect of birthing alone, “it was just mayhem,” said Susanrachel “Birdie” Condon, the other half of River and Mountain Midwives and the Hudson Valley Regional Representative on the board of the NYS Association of Licensed Midwives. “Because your doula can’t come, your spouse can’t come, nobody can come, and you’re going to be alone – and you might be separated from your baby,” she said.
On March 21, Governor Cuomo issued an executive order to allow one support person, who doesn’t have a fever, to stay with the laboring mom in the hospital. “Once I heard that, we were like, we’re not changing our plan again. Let’s just stick with the homebirth,” said Azzi. “It was kind of the push that we needed.”
Azzi, 32, happens to be the ideal candidate for a homebirth. She’d had her son, now 5, and her daughter, 21 months, without anesthesia. Working with her doula, she’s been listening to meditative recordings that help “re-train your brain to not be scared of giving birth. During birth I listen to it. It keeps me in a really calm state of mind.” Crucially, though hardest to pin down: she was already open to homebirth before the pandemic came to town. “I had this gut mama instinct,” she said. “I could not drop the thought of a home birth. I even had several dreams” about it.
Even in this best-case scenario, switching to a homebirth at the eleventh hour is stressful for everyone involved. “To be that close to birth and have everything change out from under me... I’m a planner, I’m a huge planner,” said Azzi, a full-time mom and part-time Mary Kay representative.
All of a sudden, 40 weeks of work are compressed into a frenzy of preparation, from the mundane (dealing with insurance, getting together towels and energy drinks and hydrogen peroxide) to the fundamental (building a relationship with your midwife, developing confidence in your body’s ability to have a baby without drugs).
“It’ll be good for the baby book,” said Azzi, weighing whether she wanted to be featured. “It’ll be quite a birth story.”
Then there are the women whose pregnancies do not check all the “perfect homebirth” boxes. Those who are pregnant for the first time, or who live in a house with lots of other people, who have their heart set on an epidural, who have had a C-section with no subsequent vaginal birth (VBAC), the list goes on. In normal times these are people that midwives relish working with – that’s why they became midwives. And even now, they are finding ways: Rannestad, for instance, is planning to have a woman who lives with 11 other people deliver her baby in Rannestad’s own home. A midwife in the Capitol region is renting a “safehouse” through Airbnb where women who were planning on hospital births can come to have their babies and stay for postpartum care, something that Condon is also considering “if the curve doesn’t flatten pretty soon.”
But they can’t take everyone. Midwives everywhere are having to gut check themselves to find their own answers, figure out their own limits. They have to weigh the desire to help these “last-minute Lulus,” as Condon has taken to calling them, against the obligations they have to their scheduled clients, to their families, to their own sanity. In an ironic about-face, the woman-centric advocates who have spent their careers assuaging fears about home birth are now having to say, for everyone’s safety: You’d be better off at the hospital.
“People who aren’t prepared, who don’t have relationships with the midwives, who are anticipating the option of medical support and anesthesia, they’re just ill prepared for the amount of work that it is to create a safe home birth situation,” said Condon. “The people who afraid are more likely to end up in the hospital anyway, and then we’ve created all these additional layers of chaos. It’s not the best thing for anybody.”
Is it hard to say no? “Not as hard as you’d think,” said Condon. “I’ve been a midwife for 22 years, I’ve been going to births for 26 years. Susan and I have gotten to the point where after a combined practice of 50-something years we just have to acknowledge that we can’t help everybody.”
Each new client a midwife takes on is a major investment of time – they make multiple home visits; appointments last 45 minutes – and emotional energy. But now, stretching the client load also comes with increased risk that the midwife will be infected with the virus, particularly since she can’t know for sure how rigorously latecomers have been self-quarantining. In the best case scenario, getting sick would require a midwife to hand off her entire caseload to other midwives, which they have agreed to do for one another. In the worst case, it could result in her unwittingly bringing the virus into house after house after house.
Plus, everything is just harder right now. Homebirth midwives are famous for making it up steep icy driveways in the middle of the night in beaters with hundreds of thousands of miles on them – now they have to do all that and arrive inside the house in masks and gloves and clothes that are somehow uncontaminated by the world at large.
“I just did a birth last week in a log cabin in the middle of woods,” said Condon, a mother of three. “And everyone’s talking about you know, when you get there you bring your stuff into the garage and you change your clothes before you go in the house. There’s no garage. This is a log cabin in the woods. I’m gonna change in my car. I pushed my seat back, I put a towel down on my seat that came from the clean box. I put on my scrubs, and I ran barefoot in the snow to their house. You know, my car could be contaminated if anybody has ridden in my car in the last two weeks, and touched a button at the supermarket without a glove on. It’s nuts.”
Mobile, agile and accustomed to improvising, homebirth midwives may be the medical professionals best suited for times like these. It’s a hard-earned badge and midwives tend to wear it proudly.
“I could meet somebody for the first time when I walk into the room and she’s eight centimeters dilated, she’s getting a little scared, she’s in transition,” said Condon. “You give me eight minutes and I’m her midwife. I can do that, I have that capacity. If we were in a disaster, if I was in an earthquake in Haiti, I could be anybody’s midwife. Give me eight minutes and I’m in love. But it’s not the ideal.”
----------------------------
Like first responders across the board, midwives are in severe short supply. In addition to appealing to all health care workers to volunteer their services, Governor Cuomo is temporarily allowing any midwife licensed in North America to practice in New York regardless of whether they have a state license. Some New Jersey midwives – previously limited to junior midwife status in New York – are rolling up their sleeves. Some happily retired midwives are coming out of retirement for 2020. Others are saying, Hang on a sec.
“You know, I was in midwifery to answer the call,” said Jessica Lawlor, one of the two first homebirth midwives licensed in New Jersey. “All of a sudden there’s this big call for people that need to make a different choice.” Please come out of retirement, friends begged. Could you consider just doing this?
She spent 24 hours considering. (In another ironic twist, she would finally be allowed to midwife in New York, something she’d long fought for). “I would have considered it if I wasn’t doing a significant amount of overnight shifts and doing calls for St. Anthony’s,” she said. “The clear answer was no, there’s plenty of other work.”
Lawlor, who lives in Wantage, NJ, retired her midwifery practice in 2017. Now she’s a labor and delivery nurse at St. Anthony Community Hospital, and is involved in international midwifery projects.“I was on call 24/7 for 20 years, sometimes with a caseload of 10 births per months, and raising my kids. To do that, and do that well, you just can’t expect to do it for long,” she said.
“The majority of midwives are really heart-centric people who want to help,” Lawlor said. But when you get past the emotional tug-of-war, “the next thought is whoa, wait a minute.”
Midwives across the region have been meeting and talking (virtually of course), developing screening protocol and hammering out the logistics of subbing for one another. They’re also having sobering conversations about what it will look like to "take on this many people this late in the game,” Lawlor said. “It’s probably not gonna look good.”
Yes, it’s gratifying to finally get the respect they’ve been struggling for all these years, even if it’s to be called upon to risk their lives en mass. “The nature of our jobs is that we cannot socially distance. The reality is that some of us will become ill during this time,” wrote midwife Robina Khalid, in an open letter to the birth community on behalf of the New York Home Birth Collective on March 18.
“While homebirth midwives support every birthing person’s ultimate autonomy in choosing the birth space and attendant that feels safest to them, we also have reservations about the practice of ‘birthing in place,’” Khalid wrote.
“Birthing in place” is a nickname coined by midwives to describe this brand new phenomenon. “Because ‘home birth’ is a whole thing, it’s a whole paradigm, it’s a whole relationship,” said Condon. “And if you’re someone who’s had care from an OB-GYN for 38 weeks and then you’ve decided to not go to the hospital, it’s not the same.”
“We rely on homebirth being safe because we’ve invested nine months with these people and they have a lot of education around what to expect,” said Lawlor. “They’re extremely motivated for a homebirth and they feel in their heart it’s the safest place for them to give birth. When you switch that construct and all of sudden it’s people that are running to you because they’re afraid of the other, it sets up so many unknowns and so many possibilities for failure.”
If you were to transfer into the hospital during labor (which about 10 percent of first-time mothers do), your midwife would have to do something that goes against everything their model of care is about: She would have to drop you at the hospital door. Only one person is allowed to go in with you. Now you and your partner are in the hospital alone and in crisis, which is of course worse than having gone to the hospital, calmly and voluntarily, in the first place.
“While I would never tell midwives you shouldn’t take any of these people, just be really, really, really specific about who you say yes to,” Lawlor advises. “Because you just might not really be helping, in the long run.”
That said, everyone has their inner-inner circle. “I’ve told some people that I know their background really well,” said Lawlor, “I have definitely told them if things get crazy they can, of course, think of me in an emergency situation.”
----------------------------
Last Friday morning, Cara Mulhahn, who has run her one-woman midwife operation in New York City since 1996, caught her second baby of the week. One was a first baby, whose mother had scheduled her home birth from the beginning. The other was a third baby, whose mother had been referred to Mulhahn by her doula a week and a half earlier.
In years past, Mulhahn used to take on up to 10 births a month; these days she aims for between four and six, though she’s thinking about stretching to seven. While some midwives have drawn a bright line around coronavirus hot spots, she is continuing to serve her ultra-Orthodox clients in Crown Heights and Williamsburg. On her last home visit to a mom due this month, “her kids were all in another room coughing. So that’s someone where I’ll be thinking about it more,” said Mulhahn, who wears an N95 mask and gloves and two layers of clothes, one of which she strips off post-visit and puts in a plastic bag, changing somewhere discreet, like maybe an apartment hallway, she laughs.
“Other people get the flu, they get everything, and I never get anything, so I’m not really living in fear of COVID,” she said. She once caught a baby whose mom was HIV-positive, and “frankly that was more nerve-wracking than delivering COVID,” she said. “The truth is I really like a challenge. I would say that an archetypal part of my psychological identity is to be a service person. So I feel like I’m at my best when I can be available for people.”
When we caught up with Mulhahn, she was caffeinating after a nap. That morning’s birth was “completely smooth and uncomplicated,” she said, but the hiccups that occurred, while minor, illustrate the problems that arise when a midwife and her client are essentially strangers. The woman’s water broke two weeks before her due date, and contractions didn’t follow immediately. Normally, Mulhahn would have waited until she started having regular, strong contractions to go over to her apartment. But because they'd never met, Mulhahn went over that morning, listened to the baby, took vitals, and went home. That afternoon, the woman called, concerned: she couldn’t feel the baby move.
So Mulhahn went back over at 4 p.m., putting on her two layers, mask and gloves, and had the mom eat something and listened to the baby’s heart rate: all good. The baby came the next morning – which meant that Mulhahn was handling this labor on and off for 24 hours, as opposed to a few hours that it would likely have taken if they’d had a rapport.
“If that had been my patient for the first nine months of pregnancy, I know she wouldn’t have had that concern. She got, you know, overly concerned, because I think she hadn’t planned on this choice,” Mulhahn said. “When someone’s going to switch last moment, it’s often their psyche hasn’t completely wrapped around this. They’re feeling relieved, but then once it gets started they’re like, hey wait a minute, this wasn’t my plan.”
For midwives everywhere, difficult decisions await. “I had a baby at home and I had a home birth midwife, so I think it’s a very intelligent solution to the pandemic that’s happening now,” said Mulhahn. “The problem is having to transfer. What that does to my patient relationship, it’s the most vulnerable moment. It really feels like a breach of integrity to take a first-time mom and to know the transfer rate is 10 percent. I don’t want to bring her the door and dump her there. That’s the reason we’re not excited about accepting first-time moms. It’s very sad, because they’re the ones who are most likely to have unnecessary interventions.”
The requests are backlogging on Mulhahn’s website, “and I haven’t even necessarily done verbal consults with everybody.” There’s one first-time mom in particular that Mulhahn – who delivered an HIV-positive mother, who is knowingly venturing into crowded apartments that she suspects contain the coronavirus – doesn’t know if she should take.
“I’m still thinking about if I would be comfortable taking her,” she said. “It’s her first baby. And I’m like ah. I don’t know what to do, because I’m conflicted.”
"If we were in a disaster, if I was in an earthquake in Haiti, I could be anybody’s midwife. Give me eight minutes and I’m in love. But it’s not the ideal.” - Susanrachel "Birdie" Condon, River and Mountain Midwives