Covid long haulers battle exhaustion — and more than a dozen other symptoms
Health. Local residents are plagued by lingering symptoms, ranging from heart palpitations and trouble breathing, to brain fog and loss of taste and smell.


The Rev. Dr. Rhonda Myers, a pastor at First Presbyterian Church in Goshen, N.Y., said she used to wake up in the morning excited to get up and get on with her day.
“Now,” she said, “I kind of have to convince myself to get on with my day, and that’s frustrating.”
Myers first got sick this past Christmas. Over six weeks later, she was still battling migraines and fatigue. “It’s been very slow in getting back to a sense of feeling like myself again,” she added.
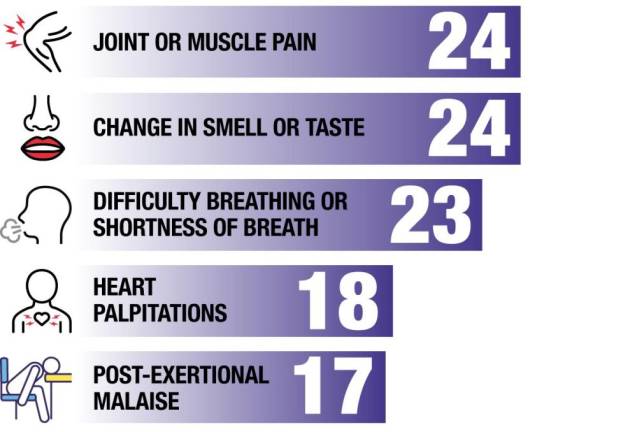
Myers is among the 10% to 50% of individuals whose initial recovery was not the end of the story, studies show. They went on to experience new, returning, or ongoing symptoms four or more weeks after being infected, a condition known as long Covid. Symptoms can be mental, physical, or both. The U.S. Centers for Disease Control lists more than 15 ailments, with varying recovery times, associated with long Covid.
“We definitely have patients who recover fully fairly quickly, you know?” said Dr. Federico Cerrone, co-medical director of Atlantic Health’s Covid Recovery Center. “In six to eight weeks, they’re fine, and they don’t need us.”
But they also have a small group of patients with persistent symptoms. And for yet another group, “its like a rollercoaster,” Cerrone said. “They seem to get better, and then they have some relapses.”
‘This was extreme’
Sparta, N.J., resident Jill Tunkavige was diagnosed with Covid-19 in December 2020. At first, she was bedridden with exhaustion and a headache.
Her sense of taste and smell also faded. This was not as debilitating as the fatigue, which she experienced in waves for about three weeks after her initial infection.
The fatigue finally subsided — but then came the daily heart palpitations. That continued for at least a month.
“This was extreme,” Tunkavige said. “I was having them all day long.”
She saw a cardiologist, who told her that the palpitations were likely Covid-related, and to just wait it out.
It took more than a year for her sense of taste to return to normal. From the time she was diagnosed, up until about two months ago, tortilla chips tasted like cardboard. “It was really weird,” she said.
Her sense of smell is still not totally back. Chicken, kitty litter, and coffee all have the same, indistinguishable scent.
“For some reason chicken just smells...weird,” she said. “It’s hard to describe. I don’t smell chicken, I just smell this weird smell. It’s just very odd.”
Exhaustion
Middletown Medical started treating post-Covid patients shortly after the first wave, approximately 18 months ago. Dr. Raj Gulati, its founder and medical director, said neurological symptoms such as the loss of taste and smell tend to linger the longest.
But, he said, “one of the biggest symptoms is chronic fatigue.”
In our newspaper’s survey of more than 180 readers who tested positive for Covid-19, 44% identified as long haulers, with fatigue the most commonly reported symptom.
Patricia Wenzel of West Milford, N.J., battled exhaustion, a lingering cough, brain fog, and trouble sleeping for more than six weeks.
“I don’t know how else to explain it. I was exhausted,” said Wenzel. “And it got to the point where I couldn’t go for a walk down the block. If I got up and put a load of wash in, I had to go back to bed.”
Myers, too, described trouble completing chores. “Even simple things, like unloading the dishwasher, I have to say to myself, ‘Ok kiddo, you can do this.’”
The mental toll
For many, the effects of long Covid go beyond physical health. Suffering fatigue for months on end exasperates anxiety and depression, said Melissa Varcardiponi, a licensed clinical social worker and founder of Counseling in Comfort in Sparta, N.J.
“What we’re finding is, it’s impacting more psycho-social stressors in one’s life,” she said. “Meaning, it’s impacting their job, it’s impacting their household, its impacting their relationship, its impacting their ability to financially keep up, on top of the stress that their health is not okay.”
In treating the fatigue, anxiety, depression, and so-called brain fog, Varcardiponi helps patients adjust their lifestyle to compensate for their changed energy levels and abilities.
“A lot of that has to do with asking for help from people in their extended family that they never would, or hiring extra support to help them at home, or helping them realize they can’t spend as much money” as they used to, if they’ve had to take a lot of extra time off because of their symptoms.
Treatment
Some of Varcardiponi’s patients who before long Covid were typically able to manage their anxiety and depression without medication ended up being referred to psychiatrists for medication evaluations because they “weren’t able to get out of that fog,” she said.
Some providers, including Atlantic Health and Middletown Medical, have established treatment centers for long haulers. There is no one-size-fits-all treatment plan. Instead, individual symptoms are treated as needed.
For many patients, having the option to see a health care provider for long Covid is a relief in itself.
“I do feel that patients have a sense of relief when they realize that this is a real thing, and that symptom normalization helps them,” said Dr. David Sousa, co-medical director of Atlantic Recovery Center with Dr. Cerrone.
Many have been told their ailments are just stress, or even made up. “They’re thankful that people are listening to them, and that they can talk to other people in our peer support groups who are experiencing the same thing,” Cerrone said. “They’re thankful that there’s some place to go.”
Tunkavige is still waiting for her sense of smell to return. But otherwise, she’s back to normal.
Myers sought help from a neurologist to manage her migraines.
And after getting weeks and weeks of rest, Wenzel said “I’m doing better than I was. Thank God.”







